Yeast Infection
Published: 14 June 2016 (Tue)
Last Updated: 17 November 2023 04:30 AM (GMT+8)

Bahasa Melayu : not_available / Malayalam : not_available / Telugu : సిలాంబం / Français : not_available
Yeast Infection Treatment
Yeast Infection (Thrush): • Yeast infection is commonly known as thrush • It can affect any part of the body, but it primarily affects: o Under arms o Area between toes o Genital area • This condition affects both men and women • Women usually develop this infection in their vagina Symptoms to look for: • Itching • Discomfort during intercourse • Burning sensation during urination Causes: • Yeast are microorganisms which are present in our body. An increase in the level of yeast leads to this infection. The level of acid, which keeps yeast in check, dips during: o Pregnancy o Menstruation o Diabetes o Intake of birth control pills Natural home remedy using aloe vera: 1. Aloe vera gel is very effective 2. Take an aloe vera leaf 3. Peel off the skin 4. Extract the gel from inside 5. Apply this gel on the infected area 6. Leave it for 30 min 7. Wash it off with water 8. Do this twice a day Natural home remedy using coconut/cinnamon oil: 1. Apply coconut or cinnamon oil 2-3 times a day 2. Both oils have anti-fungal properties Natural home remedy using yogurt: 1. Soak cotton in yogurt 2. Apply it on the infected area 3. Leave it for 30 min 4. Do this twice a day Tips: • For non-vaginal infections, apply garlic paste directly on the infected parts • Do not scratch the infected areaYeast Infection (Candidiasis) - Home Remedy & Natural Treatment
Candidiasis, commonly referred to as Yeast Infection is a kind of fungal infection caused by a kind of fungus with the scientific name ‘Candida albicaus’. With moisture and warmth aiding their survival, yeast infection generally affects body parts prone to the similar conditions. Generally affecting parts such as vulva, vagina and oral cavity; dentures, folds underneath the breasts and that of the lower abdomen may be similarly infected. Besides pregnancy and pre menstrual hormonal changes, physiological conditions affecting immune system and medications in form of steroid are some causes leading to yeast infection.
Though mostly affecting females, there are yeast infections affecting males and children as well. Marked by itching and burning sensations, there are medical curatives available to counter yeast infection. Certain homemade solutions can not only help to counter the extent of infection; but also help control its menacing impacts.
Home Remedies for Vaginal Yeast Infection
Given below are some effective yeast infection home remedies. These are natural treatment for yeast infection to reduce the infection and provide relief.
■ Friendly bacteria in non sweetened yogurt serve to counter yeast infection. One can buy ‘fitness curd’ from the market or make use of a yogurt maker to have it home made. Yogurt which can be taken as a food intake, in form of butter milk can substantially counteract infection. It can also be applied topically with tampon. Regular intake of non sweetened curd helps to destroy the harmful bacteria and fungal content of the system. External application of yogurts should be wiped out after some time.
■ Inserting a clove of garlic or tablet containing the same is also another effective home remedy. To be inserted after every two to three hour, garlic with its desired natural contents serves as an antidote to yeast infection. Garlic not only strengthens the auto immune system, but also acts as an antiseptic. Its anti fungal properties help substantially to fight against fungal base of the yeast infection.
■ Black walnut which is scientifically known as ‘Juglans nigra’has an important anti fungal element in its ‘juglone’. With this anti fungal content it serves to safe guard against long term infection caused by Candida.
■ Herbal concoction made out of one ounce of walnut tincture, with half ounce of lavender tincture and that of ten drops of tea oil is also known to inhibit yeast infection with its anti fungal mechanism. Two to three droppers of the resulting mixture may be taken regularly to counteract its effects and possibility.
■ Ten to twelve ounces of water helps counteract yeast infection by detoxifying the body. It is also prescribed by medical practitioners along with course in anti biotins.
■ Oil made out of Oregano herbal extract may help by giving the body due potency against yeast infection. The carvacrol content of oregano helps to kill yeast infection.
■ Bathing in luke warm water with drops of cider vinegar, with particular emphasis on flushing the affected areas with the same will not only prove to be relaxing, but will also help reduce the burning sensation by killing the yeast.
■ For yeast infection affecting mouth and dentures thorough rinsing with warmly salted water acts as a natural disinfectant.
■ Rinsing of mouth with disinfectant dyes available in medical stores is also one of the effective remedies.
■ Douching with yogurt solution or that containing cider vinegar may also be resorted to for countering yeast infection. Adequate care should be taken to disinfect the constituent parts of the equipment to be used in douching including container, tube and the nozzle.
■ Application of honey to the affected area and having the same rinsed with luke warm water is another of the natural home remedial options.
■ Drinking a solution containing water apple vinegar can also be an accessible option. It is one of the best possible options as it helps restoring the bacterial balance in a physiological system, besides boosting its auto immune mechanism.
■ Chances of yeast infection can be substantially reduced by avoiding stuffs like sugar, coffee and alcoholic drinks. With known affinity of yeast with sugar, eatables based on sugar should also be avoided.
■ In place of beverage rich in caffeine content, herbal tea may be opted for to mitigate the chances of yeast infection. With its medicinal property it also helps alleviate the painful effects of yeast infection.
■ Commonly affecting the vaginal areas, yeast infection is marked by disgustingly foul smelling vaginal discharge. To counteract the possibility of such an infection tightly fitted under wears or trousers should also be avoided. Clothing with tight fitting adds to the warmth which in turn encourages yeast infection. Care should be taken to disinfect the clothes used by an infected person. Similarly one should insist on using cotton underwear making room for sufficient breathing of body parts. Synthetic under wears by trapping moisture and warmth contributes to the growth and survival of yeast.
■ Last but not the least, factors which weaken auto immune system of a human body, including birth control pills and anti biotins should be avoided to ensure an effective defense against yeast infection.
| Candidiasis | |
|---|---|
| Classification and external resources | |
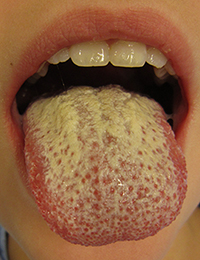
Oral candidiasis (thrush) | |
| ICD-10 | B37 |
| ICD-9 | 112 |
| DiseasesDB | 1929 |
| MedlinePlus | 001511 |
| eMedicine | med/264 emerg/76 ped/312derm/67 |
| MeSH | D002177 |
Candidiasis or thrush is a fungal infection (mycosis) of any species from the genus Candida (one genus of yeasts). Candida albicans is the most common agent of Candidiasis in humans. Also commonly referred to as a yeast infection, candidiasis is also technically known as candidosis, moniliasis, and oidiomycosis.
Candidiasis encompasses infections that range from superficial, such as oral thrush and vaginitis, to systemic and potentially life-threatening diseases. Candida infections of the latter category are also referred to as candidemia and are usually confined to severely immunocompromised persons, such as cancer, transplant, and AIDS patients, as well as nontrauma emergency surgery patients.
Superficial infections of skin and mucosal membranes by Candida causing local inflammation and discomfort are common in many human populations. While clearly attributable to the presence of the opportunistic pathogens of the genus Candida, candidiasis describes a number of different disease syndromes that often differ in their causes and outcomes.
Classification
Candidiasis may be divided into the following types:
- Mucosal candidiasis
- Oral candidiasis (thrush, Oropharyngeal candidiasis)
- Pseudomembranous candidiasis
- Erythematous candidiasis
- Hyperplastic candidiasis
- Denture related stomatitis-candida organisms are involved in about 90% of cases
- Angular stomatitis-candida organisms alone responsible for about 20% of cases, mixed infection of C. albicans and Staphylococcus aureus for about 60% of cases.
- Median rhomboid glossitis
- Candidal vulvovaginitis (vaginal yeast infection)
- Candidal balanitis, infection of the glans penis, almost exclusively occurring in uncircumcised males.
- Esophageal candidiasis (Candid esophagitis).
- Oral candidiasis (thrush, Oropharyngeal candidiasis)
- Cutaneous candidiasis
- Candidal intertrigo
- Candidal paronychia
- Perianal candidiasis
- Candidid
- Chronic mucocutaneous candidiasis
- Congenital cutaneous candidiasis
- Diaper candidiasis
- Erosio interdigitalis blastomycetica
- Invasive candidiasis
- Systemic candidiasis (one organ system involved)
- Disseminated candidiasis (multisystem involvement, e.g. "hepatosplenic candidiasis", which sometimes follows neutropenia; or "candidemia", a form of septicemia).
Antibiotic candidiasis (iatrogenic candidiasis)
Signs and symptoms
Symptoms of candidiasis vary depending on the area affected. Most candidial infections result in minimal complications such as redness, itching and discomfort, though complications may be severe or even fatal if left untreated in certain populations. In immunocompetent persons, candidiasis is usually a very localized infection of the skin or mucosal membranes, including the oral cavity (thrush), the pharynx or esophagus, the gastrointestinal tract, the urinary bladder, or the genitalia (vagina, penis).
Candidiasis is a very common cause of vaginal irritation, or vaginitis, and can also occur on the male genitals. In immunocompromised patients, Candida infections can affect the esophagus with the potential of becoming systemic, causing a much more serious condition, a fungemia called candidemia.
Thrush is commonly seen in infants. It is not considered abnormal in infants unless it lasts longer than a few weeks.
Infection of the vagina or vulva may cause severe itching, burning, soreness, irritation, and a whitish or whitish-gray cottage cheese-like discharge, often with a curd-like appearance. These symptoms are also present in the more common bacterial vaginosis. In a 2002 study published in the Journal of Obstetrics and Gynecology, only 33% of women who were self-treating for a yeast infection actually had a such an infection, while most had either bacterial vaginosis or a mixed-type infection. Symptoms of infection of the male genitalia include red, patchy sores near the head of the penis or on the foreskin, severe itching, or a burning sensation. Candidiasis of the penis can also have a white discharge, although uncommon.
Perianal candidiasis can cause pruritis ani. The lesion can be erythematous, papular or ulcerative in appearance, and it is not considered to be a sexually transmissible disease.
Esophageal candidiasis can cause dysphagia (difficulty swallowing), or less commonly odynophagia (painful swallowing).
Causes
Candida yeasts are generally present in healthy humans, particularly on the skin, but their growth is normally limited by the human immune system, by competition of other microorganisms, such as bacteria occupying the same locations in the human body, and in the case of skin, by the relative dryness of the skin, as Candida requires moisture for growth.
C. albicans was isolated from the vaginas of 19% of apparently healthy women, i.e., those who experienced few or no symptoms of infection. External use of detergents or douches or internal disturbances (hormonal or physiological) can perturb the normal vaginal flora, consisting of lactic acid bacteria, such as lactobacilli, and result in an overgrowth of Candida cells, causing symptoms of infection, such as local inflammation. Pregnancy and the use of oral contraceptives have been reported as risk factors. Diabetes mellitus and the use of antibacterial antibiotics are also linked to an increased incidence of yeast infections. Diets high in simple carbohydrates have been found to affect rates of oral candidiases, and hormone replacement therapy and infertility treatments may also be predisposing factors. Wearing wet swimwear for long periods of time is also believed to be a risk factor.
A weakened or undeveloped immune system or metabolic illnesses such as diabetes are significant predisposing factors of candidiasis. Diseases or conditions linked to candidiasis include HIV/AIDS, mononucleosis, cancer treatments, steroids, stress, and nutrient deficiency. Almost 15% of people with weakened immune systems develop a systemic illness caused by Candida species. In extreme cases, these superficial infections of the skin or mucous membranes may enter into the bloodstream and cause systemic Candida infections.
In penile candidiasis, the causes include sexual intercourse with an infected individual, low immunity, antibiotics, and diabetes. Male genital yeast infections are less common, and incidences of infection are only a fraction of those in women; however, yeast infection on the penis from direct contact via sexual intercourse with an infected partner is not uncommon.
Candida species are frequently part of the human body's normal oral and intestinal flora. Treatment with antibiotics can lead to eliminating the yeast's natural competitors for resources, and increase the severity of the condition. In the Western Hemisphere, about 75% of females are affected at some time in their lives.
Diagnosis
Diagnosis of a yeast infection is done either via microscopic examination or culturing.
For identification by light microscopy, a scraping or swab of the affected area is placed on a microscope slide. A single drop of 10% potassium hydroxide (KOH) solution is then added to the specimen. The KOH dissolves the skin cells, but leaves the Candida cells intact, permitting visualization of pseudohyphae and budding yeast cells typical of many Candida species.
For the culturing method, a sterile swab is rubbed on the infected skin surface. The swab is then streaked on a culture medium. The culture is incubated at 37°C for several days, to allow development of yeast or bacterial colonies. The characteristics (such as morphology and colour) of the colonies may allow initial diagnosis of the organism causing disease symptoms.
Treatment
Candidiasis is commonly treated with antimycotics; these antifungal drugs include topical clotrimazole, topical nystatin, fluconazole, and topical ketoconazole.
Localized infection
A one-time dose of fluconazole is 90% effective in treating a vaginal yeast infection. Local treatment may include vaginal suppositories or medicated douches. Other types of yeast infections require different dosing. Gentian violet can be used for thrush in breastfeeding babies, but when used in large quantities, it can cause mouth and throat ulcerations, and has been linked to mouth cancer in humans and to cancer in the digestive tract of other animals. C. albicans can develop resistance to fluconazole, this being more of an issue in those with HIV/AIDS who are often treated with multiple courses of fluconazole for recurrent oral infections.
There is not enough evidence to determine if probiotics (either as pills or as yogurt) has an effect on the rate of occurrence of vaginal yeast infections. No benefit has been found for active infections.
Blood infection
In candidial infections of the blood intravenous fluconazole or an echinocandin such as caspofungin may be used. Amphotericin B is another option.
Prognosis
Among individuals being treated in intensive care units, there is a mortality rate of about 30-50% when systemic candidiasis develops.
Epidemiology
In humans, oral candidiasis is the most common form of candidiasis, by far the most common fungal infection of the mouth, and it also represents the most common opportunistic oral infection in humans.
Esophageal candidiasis is the most common esophageal infection in persons with AIDS, and accounts for about 50% of all esophageal infections, often coexisting with other esophageal diseases. About 2/3 of people with AIDS and esophageal candidiasis also have oral candidiasis.
Candida septicemia is rare.
History
Descriptions of what sounds like oral thrush go back to the time of Hippocrates circa 460 - 370 BC.
Vulvovaginal candidiasis was first described in 1849 by Wilkinson. In 1875 Haussmann demonstrated that the causative organism in both vulvovaginal candidiasis and oral candidiasis was the same.
The incidence of candidiasis increased following World War II, with the advent of antibiotics, and then decreased again with the development of nystatin, introduced by Elizabeth Hazen and Rachel Brown.
The colloquial term "thrush" refers to the resemblance of the white flecks present in some forms of candidiasis (e.g. pseudomembranous candidiasis), with the breast of the bird of the same name. The term candidosis is largely used in British English, and candidiasis in American English. Candida is also pronounced differently, in American English, the stress is on the "i", whereas in British English there is no stress on the "i".
The genus Candida and species C. albicans were described by botanist Christine Marie Berkhout in her doctoral thesis at the University of Utrecht in 1923. Over the years, the classification of the genera and species has evolved. Obsolete names for this genus include Mycotorula and Torulopsis. The species has also been known in the past as Monilia albicans and Oidium albicans. The current classification is nomen conservandum, which means the name is authorized for use by the International Botanical Congress (IBC).
The genus Candida includes about 150 different species; however, only a few are known to cause human infections. C. albicans is the most significant pathogenic species. Other species pathogenic in humans include C. tropicalis, C. glabrata, C. krusei, C. parapsilosis, C. dubliniensis, and C. lusitaniae.
The name Candida was proposed by Berkhout. It is from the Latin word toga candida, referring to the white toga (robe) that was worn by candidates for the Senate of the ancient Roman republic. Albicans also comes from Latin, albicare meaning "to whiten." These names refer to the generally white appearance of Candida species when cultured.
Society and culture
Some alternative medicine proponents postulate a widespread occurrence of systemic candidiasis (or candida hypersensitivity syndrome, yeast allergy, fungal type dysbiosis or gastrointestinal candida overgrowth), a medically unrecognised condition. The view was most widely promoted in a book published by Dr. William Crook that hypothesized a variety of common symptoms such as fatigue, PMS, sexual dysfunction, asthma, psoriasis, digestive and urinary problems, multiple sclerosis, and muscle pain could be caused by subclinical infections of C. albicans. Crook suggested a variety of remedies to treat these symptoms, including dietary modification (commonly referred to as the rainbow diet—eating fresh foods and avoiding foods high in vinegar, sugar, or yeast), prescription antifungals, pau d'arco tea, echinacea tea, and colonic irrigation. With the exception of the few dietary studies in the urinary tract infection section, conventional medicine has not used most of these alternatives, since there is limited scientific evidence proving either their effectiveness or that subclinical systemic candidiasis is a viable diagnosis.
In 1990, alternative health vendor Nature's Way signed an FTC consent agreement not to misrepresent in advertising any self-diagnostic test concerning yeast conditions or to make any unsubstantiated representation concerning any food or supplement's ability to control yeast conditions, with a fine of $30,000 payable to the National Institutes of Health for research in genuine candidiasis.
References
- Walsh TJ, Dixon DM (1996). "Deep Mycoses". In Baron S et al. eds. Baron's Medical Microbiology (4th ed.). Univ of Texas Medical Branch. ISBN 0-9631172-1-1.
- ^ a b c d
MedlinePlus Encyclopedia Vaginal yeast infection - ^ a b
James, William D.; Berger, Timothy G.; et al. (2006). Andrews' Diseases of the Skin: clinical Dermatology. Saunders Elsevier. pp. 308–311. ISBN 0-7216-2921-0. - ^
Kourkoumpetis T, Manolakaki D, Velmahos G, et al. (2010). "Candida infection and colonization among non-trauma emergency surgery patients". Virulence 1 (5): 359–66. doi:10.4161/viru.1.5.12795. PMID 21178471. - ^ a b c
Fidel PL (2002). "Immunity to Candida". Oral Dis. 8: 69–75. doi:10.1034/j.1601-0825.2002.00015.x. PMID 12164664. - ^ a b
Pappas PG (2006). "Invasive candidiasis". Infect. Dis. Clin. North Am. 20 (3): 485–506. doi:10.1016/j.idc.2006.07.004. PMID 16984866. - ^
Nyirjesy, P; Sobel, JD (2013 May). "Genital mycotic infections in patients with diabetes.". Postgraduate medicine 125 (3): 33–46. PMID 23748505. - ^ a b c
Yamada T, Alpers DH, et al. (2009). Textbook of gastroenterology (5th ed.). Chichester, West Sussex: Blackwell Pub. p. 814. ISBN 978-1-4051-6911-0. - ^
Errol Reiss, H. Jean Shadomy, G. Marshall Lyon (2011). "Chapter 11". Fundamental medical mycology. Hoboken, N.J.: John Wiley & Sons. ISBN 9781118101766. - ^ a b
Dolin, [edited by] Gerald L. Mandell, John E. Bennett, Raphael (2010). Mandell, Douglas, and Bennett's principles and practice of infectious diseases (7th ed.). Philadelphia, PA: Churchill Livingstone/Elsevier. pp. Chapter 250. ISBN 978-0-443-06839-3. - "Thrush". 2011. Retrieved 2011-04-08.
- Terri Warren, RN (2010). "Is It a Yeast Infection?". Retrieved 2011-02-23.
- ^
Ferris DG; Nyirjesy P; Sobel JD; Soper D; Pavletic A; Litaker MS (March 2002). "Over-the-counter antifungal drug misuse associated with patient-diagnosed vulvovaginal candidiasis". Obstetrics and Gynecology 99 (3): 419–425. doi:10.1016/S0029-7844(01)01759-8. PMID 11864668. - ^
Bruce G. Wolff et al., ed. (2007). The ASCRS textbook of colon and rectal surgery. New York: Springer. pp. 241, 242, 245. ISBN 0-387-24846-3. - ^
Mulley, A. G.; Goroll, A. H. (2006). Primary Care Medicine: office evaluation and management of the adult patient. Philadelphia: Wolters Kluwer Health. pp. 802–3. ISBN 0-7817-7456-X. Retrieved 2008-11-23. - ^
Goehring, Richard V. (2008). Mims' medical microbiology. (4th ed. ed.). Philadelphia, PA: Mosby Elsevier. p. 656. ISBN 978-0-323-04475-2. - ^
Mårdh P A, Novikova N, Stukalova E (October 2003). "Colonisation of extragenital sites by Candida in women with recurrent vulvovaginal candidosis". BJOG 110 (10): 934–7. doi:10.1111/j.1471-0528.2003.01445.x. PMID 14550364. - ^ a b
Schiefer HG (1997). "Mycoses of the urogenital tract". Mycoses 40 (Suppl 2): 33–6. doi:10.1111/j.1439-0507.1997.tb00561.x. PMID 9476502. - ^
Akpan, A; Morgan, R (2002 Aug). "Oral candidiasis". Postgraduate Medical Journal 78 (922): 455–9. doi:10.1136/pmj.78.922.455. PMC 1742467. PMID 12185216. - ^
Odds FC (1987). "Candida infections: an overview". Crit. Rev. Microbiol. 15 (1): 1–5. doi:10.3109/10408418709104444. PMID 3319417. - ^
Choo Z.W., Chakravarthi S., Wong S.F., Nagaraja H.S., Thanikachalam P.M., Mak J.W., Radhakrishnan A., Tay A. (2010). "A comparative histopathological study of systemic candidiasis in association with experimentally induced breast cancer". Oncology Letters 1 (1): 215–222. doi:10.3892/ol_00000039. ISSN 1792-1082. PMC 3436220. PMID 22966285. - ^
David LM, Walzman M, Rajamanoharan S (October 1997). "Genital colonisation and infection with candida in heterosexual and homosexual males". Genitourin Med 73 (5): 394–6. PMC 1195901. PMID 9534752. - ^
Bassetti, M; Mikulska, M; Viscoli, C (December 2010). "Bench-to-bedside review: therapeutic management of invasive candidiasis in the intensive care unit.". Critical Care 14 (6): 244. doi:10.1186/cc9239. PMID 21144007. - ^
Srikumar Chakravarthi, Nagaraja HS (2010). "A comprehensive review of the occurrence and management of systemic candidiasis as an opportunistic infection". Microbiology Journal 1 (2): 1–5. ISSN 2153-0696. - ^
Moosa MY, Sobel JD, Elhalis H, Du W, Akins RA (2004). "Fungicidal Activity of Fluconazole against Candida albicans in a Synthetic Vagina-Simulative Medium". Antimicrob. Agents Chemother. 48 (1): 161–7. doi:10.1128/AAC.48.1.161-167.2004. PMC 310176. PMID 14693534. - ^
Craigmill A (December 1991). "Gentian Violet Policy Withdrawn". Cooperative Extension University of California -- Environmental Toxicology Newsletter 11 (5). - ^
Morschhäuser, J (2002 Jul 18). "The genetic basis of fluconazole resistance development in Candida albicans.". Biochimica et biophysica acta 1587 (2-3): 240–8. PMID 12084466. - ^
Jurden, L; Buchanan, M; Kelsberg, G; Safranek, S (2012 Jun). "Clinical inquiries. Can probiotics safely prevent recurrent vaginitis?". The Journal of family practice 61 (6): 357, 368. PMID 22670239. - ^ a b
Pappas, PG; Kauffman, CA; Andes, D; Benjamin DK, Jr; Calandra, TF; Edwards JE, Jr; Filler, SG; Fisher, JF; Kullberg, BJ; Ostrosky-Zeichner, L; Reboli, AC; Rex, JH; Walsh, TJ; Sobel, JD; Infectious Diseases Society of, America (2009 Mar 1). "Clinical practice guidelines for the management of candidiasis: 2009 update by the Infectious Diseases Society of America.". Clinical infectious diseases : an official publication of the Infectious Diseases Society of America 48 (5): 503–35. PMID 19191635. - ^
Williams, D; Lewis, M (2011 Jan 28). "Pathogenesis and treatment of oral candidosis.". Journal of oral microbiology 3. PMC 3087208. PMID 21547018. - ^
Anil Ghom, Shubhangi Mhaske (2010). Textbook of oral pathology. New Delhi: Jaypee Brothers Medical Publishers. pp. 498,508–514. ISBN 9788184484021. - ^
Bouquot, Brad W. Neville , Douglas D. Damm, Carl M. Allen, Jerry E. (2002). Oral & maxillofacial pathology (2. ed. ed.). Philadelphia: W.B. Saunders. pp. 189–197. ISBN 0721690033. - ^
Lalla, RV; Patton, LL; Dongari-Bagtzoglou, A (2013 Apr). "Oral candidiasis: pathogenesis, clinical presentation, diagnosis and treatment strategies.". Journal of the California Dental Association 41 (4): 263–8. PMID 23705242. - ^
Gow, Neil (8 May 2002). "Candida albicans - a fungal Dr Jekyll and Mr Hyde". Mycologist 16 (01). doi:10.1017/S0269915X02006183. - ^ a b c d e
Lynch, DP (1994 Aug). "Oral candidiasis. History, classification, and clinical presentation.". Oral surgery, oral medicine, and oral pathology 78 (2): 189–93. PMID 7936588. - ^
Obladen, M (2012). "Thrush - nightmare of the foundling hospitals.". Neonatology 101 (3): 159–65. PMID 22024688. - ^
Scully, Crispian. "Mucosal Candidiasis (Medscape)". WebMD LLC. Retrieved 8 September 2013. - ^ a b
candidiasis hypersensitivity, National Council Against Health Fraud - ^ a b
Crook, William G. (1986). The yeast connection: a medical breakthrough. New York: Vintage Books. ISBN 0-394-74700-3. - ^
Weil A (2002-10-25). "Concerned About Candidiasis?". Weil Lifestyle. Retrieved 2008-02-21. - ^
Barrett S (2005-10-08). "Dubious "Yeast Allergies"". QuackWatch. Retrieved 2008-02-21. - ^
Katherine Zeratsky. "Candida cleanse: Does it treat candidiasis?". Mayo Clinic. Retrieved 2009-08-09. - ^
Blonz ER (December 1986). "Is there an epidemic of chronic candidiasis in our midst?" (PDF). JAMA 256 (22): 3138–9. doi:10.1001/jama.1986.03380220104032. PMID 3783850.
| |||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||